THE COURAGE TO FEEL AGAIN: THE NEUROSCIENCE OF EMOTION
BY SERGIO SHAN-LEE | TO BE MORE HUMAN
Abstract: Interoception plays a central role in emotional awareness, connecting bodily signals such as heartbeat and breath with how we experience emotion. Connecting with our emotions often means reconnecting body and mind. Recent studies show that interoception — awareness of internal signals like heartbeat and breath — shapes emotional experience. For example, fearful images are detected more quickly if shown during the heartbeat’s contraction (systole) versus relaxation (diastole)[1]. Likewise, people with higher resting heart rate variability (HRV) report better emotion regulation and clarity[2][3]. These findings suggest that the heart’s rhythms broadcast information to the brain that can amplify or dampen feelings. Therapeutic practices that foster interoceptive awareness — such as paced breathing, mindful body scans, expressive writing, and emotion-focused therapy — appear to help people access and process emotions that were previously shut down. Research on interoception shows that internal signals from the heart and body strongly influence emotional awareness. While some claims (e.g. mystical “heart coherence” effects or transplanted “memories”) lack scientific support, the core evidence encourages clinicians to guide clients in “returning to the heart” safely. This article reviews the evidence on heart-centered emotion, relevant brain mechanisms, and interventions designed to help clients rediscover the courage to feel.
INTEROCEPTION AND EMOTIONAL AWARENESS
The heart has always been a powerful metaphor for emotion, and science is increasingly giving this metaphor literal weight. Interoception research shows that physiological changes contribute directly to how we feel[4]. In everyday terms, “feeling it in your heart” means attending to your body’s signals. For instance, when you feel anxiety, you might notice a flutter in your chest or quickened breath. Emotional honesty is about noticing and interpreting these sensations rather than ignoring them. Clinicians often encourage clients to ask, “Where do you feel this in your body?” to bridge cognition and sensation. Over time, such attention can transform vague distress into meaningful emotion.
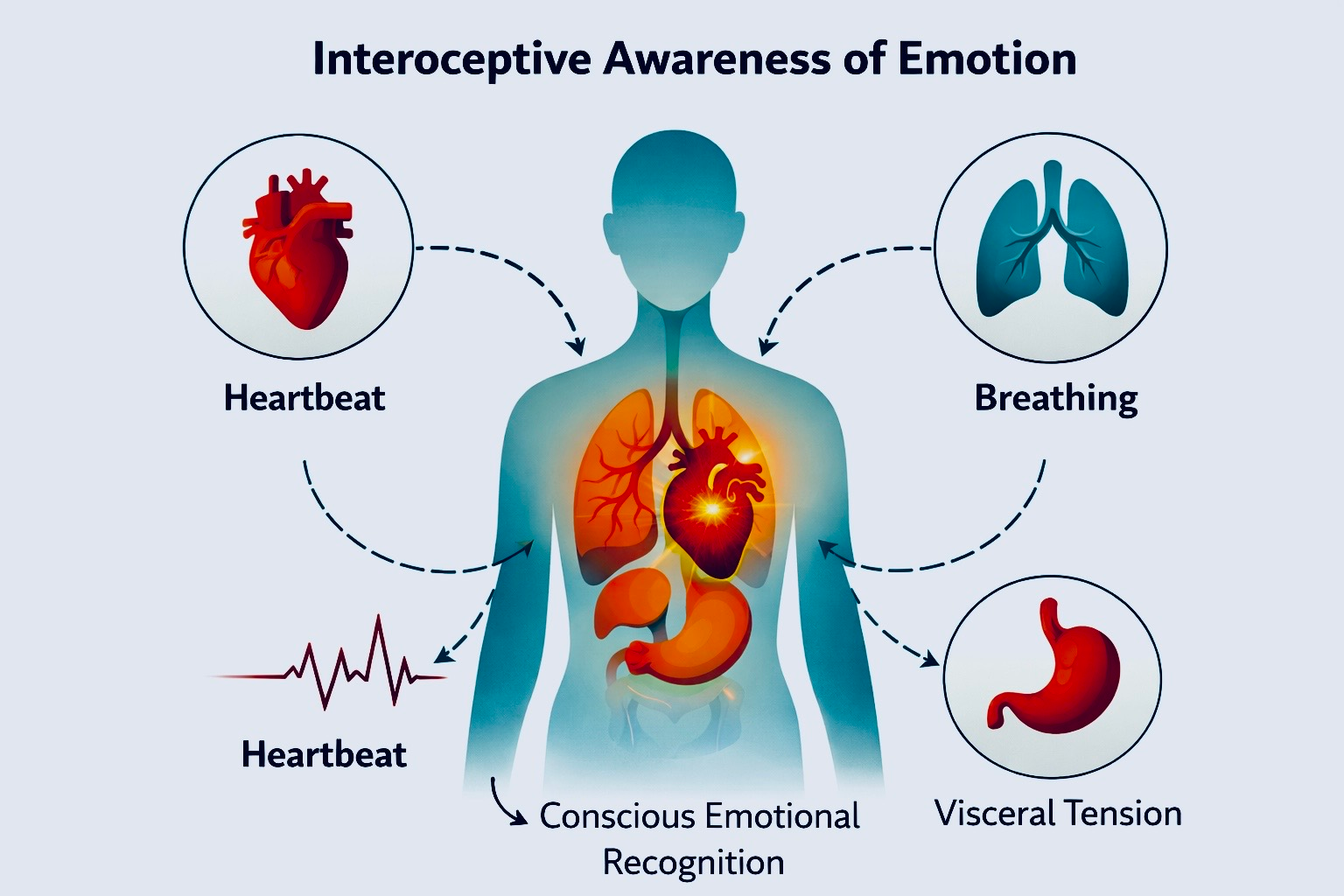
Figure 1. Interoceptive Awareness of Emotion. Emotional awareness often begins with perception of internal bodily signals such as heartbeat, breathing, and visceral tension. Research on interoception suggests that attending to these sensations helps translate physiological states into consciously recognized emotional experience.
Illustrated By To Be More Human.
Neuroscience explains this connection: the heart sends continuous feedback to the brain, and the brain interprets these signals as part of emotion. Brain regions such as the insula and anterior cingulate cortex are central to interoception, integrating bodily signals into conscious emotional experience. Key brain regions — the insula and anterior cingulate cortex (ACC) — monitor interoceptive signals. The insula integrates bodily data into subjective feeling, and the ACC evaluates how those feelings fit our goals and safety. For example, when an insula “alert” signal comes in (a fast heartbeat), the brain might label it as fear or excitement depending on context. The prefrontal cortex then helps reframe the sensation (e.g. “That quick pulse means I’m excited about this, not threatened by it”). Emotional honesty therefore involves strengthening this body–brain loop: acknowledging that a racing heart is telling you something important, and then using the mind to understand and integrate that feeling.
PHYSIOLOGICAL MECHANISMS: HOW THE HEART COMMUNICATES
The body’s pathways for heart–brain communication are well mapped. Each heartbeat stretches blood vessels, activating baroreceptors that fire signals to the brainstem via the vagus nerve[1]. Researchers have cleverly shown that these signals influence perception. In one experiment (Ozturk et al., 2025), participants viewed faces suppressed by flickering images; fearful faces synced to systole became visible faster than when synced to diastole[1]. Neutral faces showed no difference. This means that during systole — when baroreceptors fire strongly — the brain becomes briefly more sensitive to threat cues. In essence, the heart “gates” which information gets through: it momentarily boosts the processing of salient, especially threatening, stimuli[1]. This process reflects the broader heart–brain feedback loop illustrated in Figure 2.
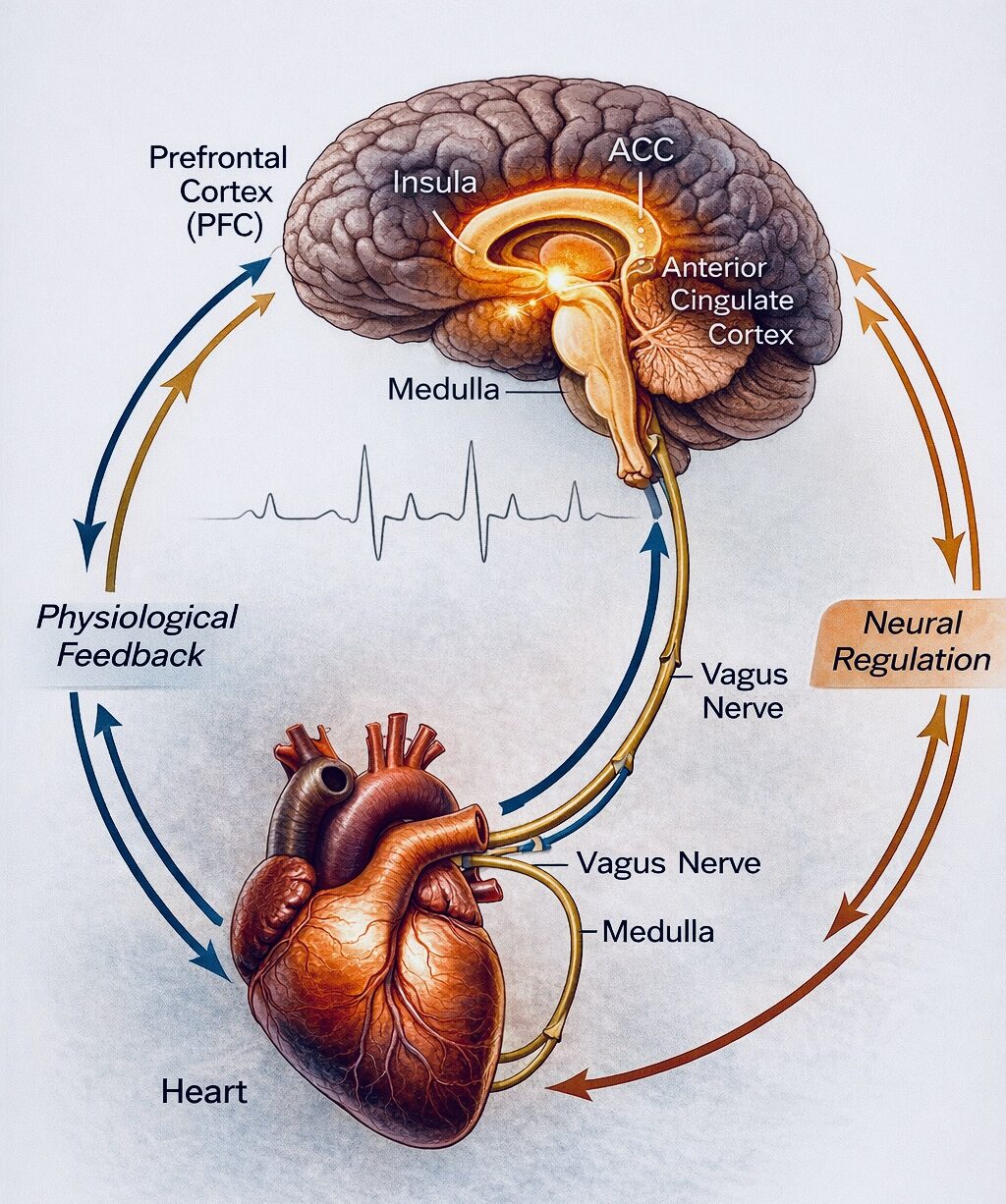
Figure 2. Heart–Brain Communication Loop. Signals from the heart travel through baroreceptors and the vagus nerve to the brainstem and cortical regions including the insula and anterior cingulate cortex (ACC). These interoceptive signals contribute to emotional awareness while the prefrontal cortex (PFC) regulates autonomic responses, forming a bidirectional physiological feedback loop between body and brain.
Illustrated by To Be More Human.
The heart also possesses its own network of neurons (the “intrinsic cardiac nervous system”) that participates in this feedback. Though sometimes romanticized as carrying memories, this cardiac network primarily modulates heart function and conveys its state to the central nervous system. For practical purposes, the key takeaway is that the heart actively signals its condition to the brain, and the brain uses this input to shape feelings. Another important concept is heart rate variability (HRV) — the natural variation in time between beats. As illustrated in Figure 3, HRV reflects the dynamic balance between sympathetic and parasympathetic activity within the autonomic nervous system.
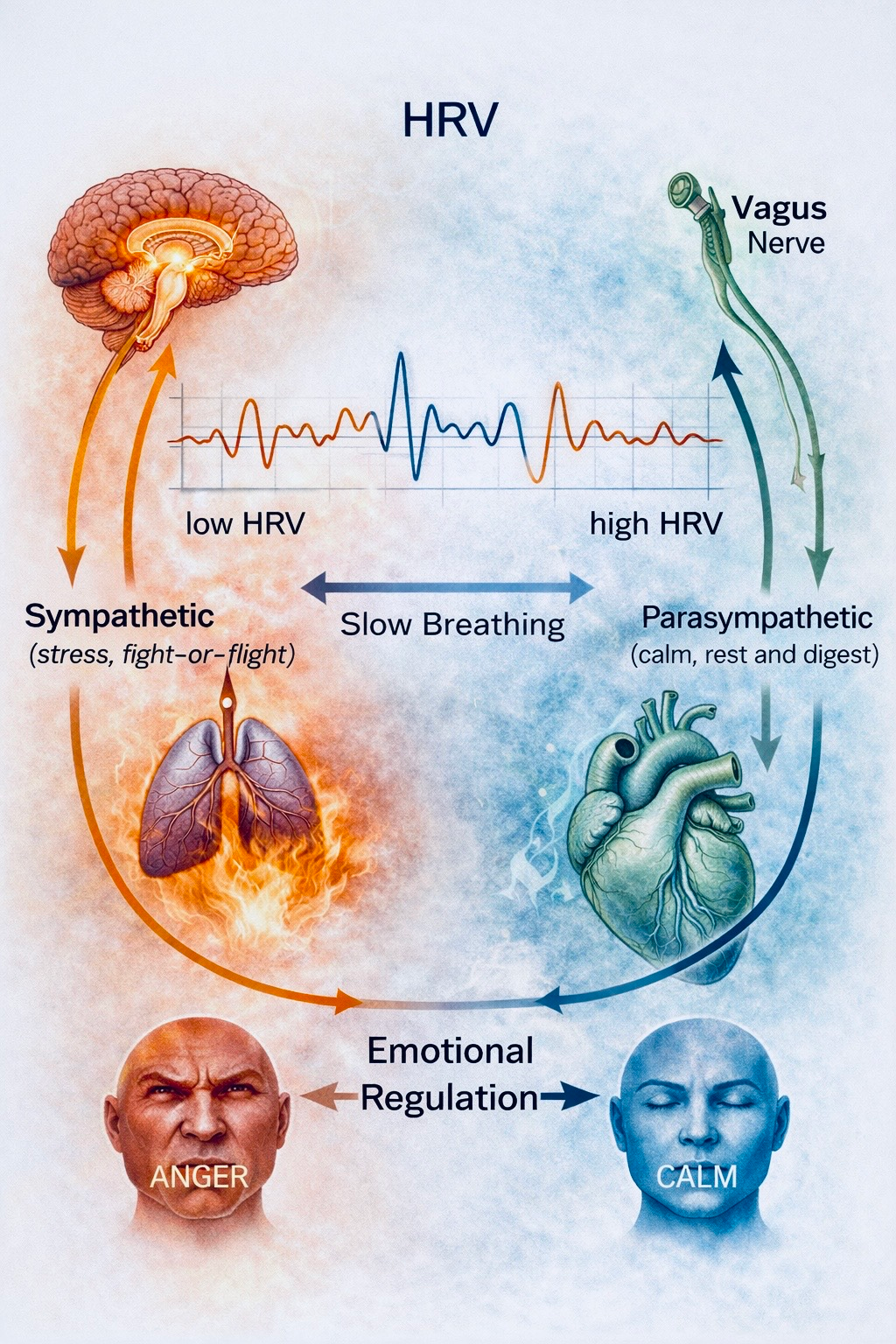
Figure 3. Heart Rate Variability and Emotional Regulation. Heart rate variability (HRV) reflects the dynamic balance between the sympathetic (stress response) and parasympathetic (rest-and-digest) branches of the autonomic nervous system. Higher HRV is associated with improved emotional regulation, resilience, and adaptive stress responses, while slow breathing practices can increase vagal activity and support emotional stability.
Illustrated By To Be More Human.
High HRV indicates a flexible, responsive autonomic system; low HRV indicates rigidity and stress. Notably, many studies link higher HRV with better emotional resilience. For example, Williams et al. (2015) found that individuals with lower resting HRV reported much greater difficulty with emotional clarity and impulse control[2]. In other words, a calm, variable heart rhythm seems to go hand-in-hand with a calm, clear mind. Therapies that increase HRV (such as slow coherent breathing) reliably reduce anxiety and support positive mood[3]. Thus, training clients to breathe in synchrony with their heartbeat (often at ~5 breaths/minute) can literally raise their physiological capacity for feeling safe.
NEURAL INTEGRATION: THE BRAIN'S ROLE
Interoceptive signals from the heart are integrated by specific brain circuits. The insula receives the raw signal and forms the basic feeling; the ACC evaluates its significance (for instance, threat versus salience); and the prefrontal cortex (PFC) interprets and regulates it. EEG and imaging studies support this. Tanaka et al. (2025) found that heartbeat-evoked potentials activate the right anterior insula and (ACC), linking them to conscious awareness of internal signals[4]. Figure 4 illustrates how regions such as the insula, anterior cingulate cortex, and prefrontal cortex translate physiological signals into emotional awareness and regulation.
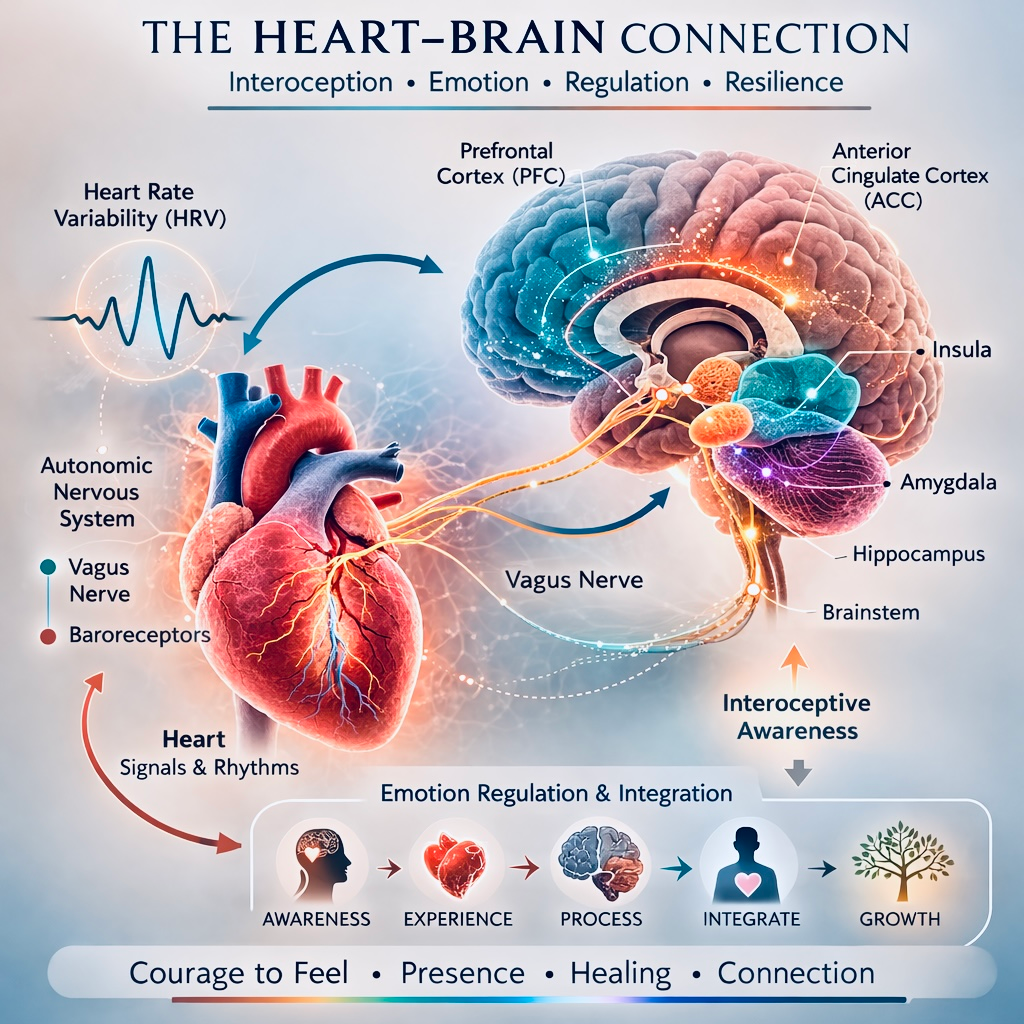
Figure 4. Neural Integration of Cardiac Interoceptive Signals. Cardiovascular signals are conveyed through the vagus nerve and brainstem to cortical and limbic structures including the insula, anterior cingulate cortex (ACC), amygdala, hippocampus, and prefrontal cortex. This neurovisceral network integrates physiological states with emotional awareness and regulatory processes.
Illustrated By To Be More Human
This network is bidirectional. The PFC can send regulatory feedback via the vagus to quiet the heart, completing a loop. For example, when a person practices calm breathing or meditation, PFC engagement can lower heart rate. Conversely, when heart signals surge (as in panic), insula and ACC drive up amygdala and brainstem activity. Trauma and dissociation highlight what happens when this loop is disrupted. Research (Leech et al., 2024) shows that PTSD patients often have diminished insula activation during interoceptive tasks[5]. In dissociative states, the system down-regulates so much that people report not even feeling their heartbeat or breath. Part of therapy, then, is carefully turning these signals back on – teaching the nervous system that interoceptive input is safe and informative, not overwhelming. High HRV often signals a well-regulated neurovisceral network; low HRV can indicate a “stuck” system that needs retraining[2][3].
NEUROVISCERAL INTEGRATION MODEL
One theoretical framework that helps explain the relationship between cardiac physiology and emotional regulation is the Neurovisceral Integration Model (Thayer & Lane, 2000; Thayer et al., 2012). This model proposes that adaptive emotional functioning depends on coordinated activity between the prefrontal cortex, limbic structures, and the autonomic nervous system, particularly through vagal pathways that regulate cardiac activity. Within this framework, the prefrontal cortex exerts inhibitory control over subcortical threat-processing regions such as the amygdala, while simultaneously influencing heart function through parasympathetic mechanisms. A key physiological marker of this regulatory capacity is heart rate variability (HRV), which reflects the dynamic balance between sympathetic and parasympathetic activity within the autonomic nervous system. Higher resting HRV has been associated with stronger functional connectivity within this regulatory network and greater flexibility in emotional responding, including improved emotional clarity, impulse control, and resilience to stress (Thayer et al., 2012). Conversely, reduced HRV is often linked to diminished regulatory capacity and increased vulnerability to anxiety, depression, and stress-related disorders. In this sense, the heart does not merely respond to emotional states; rather, it participates in a bidirectional regulatory system in which physiological signals and neural control processes continuously interact to shape emotional experience.
REFERENCES
Gerger, H., Werner, C. P., Gaab, J., & Cuijpers, P. (2022). Comparative efficacy of expressive writing for trauma: A systematic review and network meta-analysis. Psychological Medicine, 52(15), 3484–3496. https://doi.org/10.1017/S0033291721000143[6].
Leech, K. A., Stapleton, P., & Patching, A. (2024). Interoceptive awareness and PTSD: A scoping review. Frontiers in Psychiatry, 15, 1355442. https://doi.org/10.3389/fpsyt.2024.1355442[5].
Ozturk, O. C., McFadyen, J., & Azevedo, R. T. (2025). Cardiac signals facilitate emotional awareness. Psychophysiology, 62(10), e70168. https://doi.org/10.1111/psyp.70168[1].
Tanaka, Y., Ito, Y., Shibata, M., Terasawa, Y., & Umeda, S. (2025). Heartbeat-evoked potentials reflect interoceptive awareness during an emotional situation. Scientific Reports, 15, 8072. https://doi.org/10.1038/s41598-025-92854-4
Williams, D. P., Cash, C., Rankin, C., Bernardi, A., Giordano, N., & Thayer, J. F. (2015). Resting HRV predicts emotion regulation difficulties: Evidence for the neurovisceral integration model. Frontiers in Psychology, 6, 261. https://doi.org/10.3389/fpsyg.2015.00261[2].
Yarnell, S. L., et al. (2022). From dysregulation to coherence: HRV biofeedback and emotion regulation. Healthcare (Basel), 10(2), 376. https://doi.org/10.3390/healthcare10020376[3]
Thayer, J. F., & Lane, R. D. (2000). A model of neurovisceral integration in emotion regulation and dysregulation. Journal of Affective Disorders, 61, 201–216.
Thayer, J. F., Åhs, F., Fredrikson, M., Sollers, J. J., & Wager, T. D. (2012). A meta-analysis of heart rate variability and neuroimaging studies: Implications for heart–brain integration. Neuroscience & Biobehavioral Reviews, 36, 747–756.
